Conversational AI in Insurance: Claims, Service, Compliance, and Operating Priorities
Conversational AI in insurance is becoming a practical operating layer for carriers, brokers, MGAs, and service teams that need to handle more customer interactions without weakening accuracy or trust. The opportunity is not simply faster replies. The stronger use case is helping insurance companies manage loss intake, service questions, routine tasks, and spikes while keeping licensed teams focused on judgment-heavy work.
The insurance industry has always depended on trust, documentation, and timely response. Policyholders contact insurance providers when they need answers about coverage, billing, renewals, claims processing, or urgent loss events. If the experience is slow or fragmented, customer satisfaction drops quickly.
Automation can improve that experience, but only when it is connected to existing systems, trained around insurance operations, and governed with clear escalation rules. A disconnected chatbot may answer basic questions. Conversational AI solutions can support complete workflows across policy service, claims operations, customer engagement, and compliance.

What Is Insurance Conversational AI?
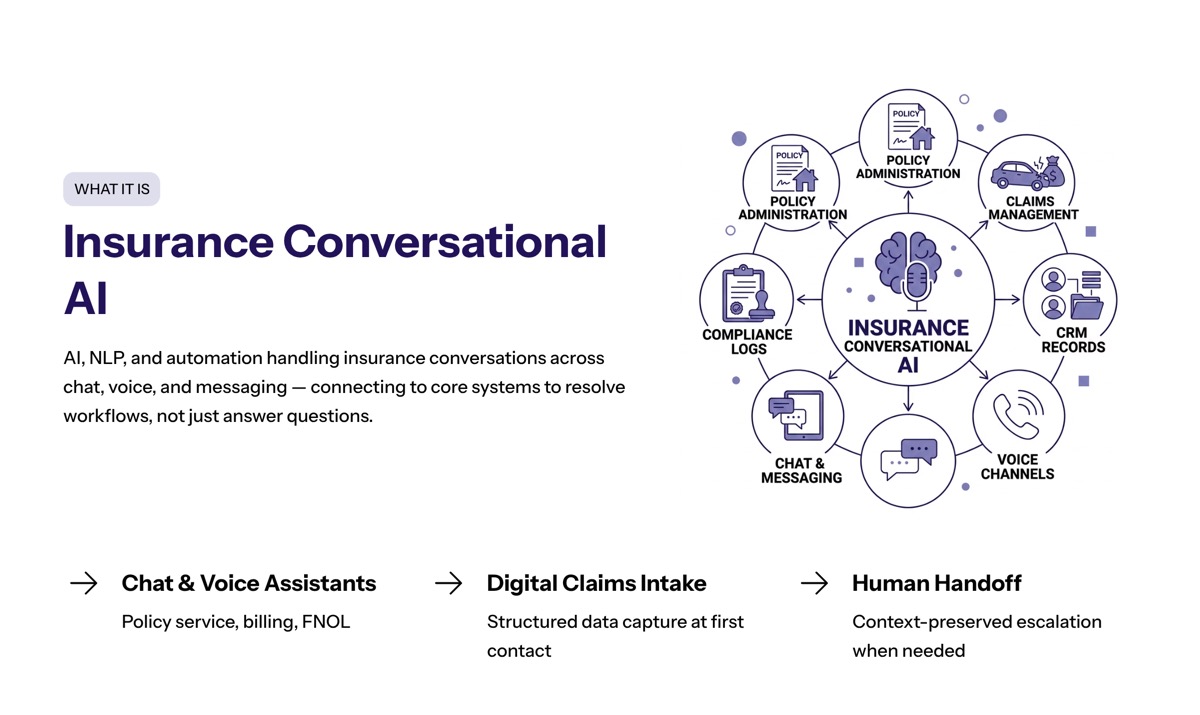
Conversational AI in insurance is the use of artificial intelligence, natural language processing, and automation to handle insurance conversations through chat, voice, messaging platforms, or embedded digital experiences. It helps systems understand customer queries, retrieve coverage information, collect structured data, and provide accurate answers. In the insurance industry, that makes service automation a data and workflow problem, not only a response-speed problem.
Insurance conversational AI can appear as chat assistants, AI voice agents, digital claims intake tools, virtual policy-service assistants, or AI agents inside service platforms. These systems may support an insurance customer through a billing question, renewal reminder, First Notice of Loss, or claim status request.
The best conversational AI does not replace human insurance agents. It handles repeatable interactions, identifies when human intervention is needed, and gives the service team better context when they take over.
How AI Works in Insurance Conversations
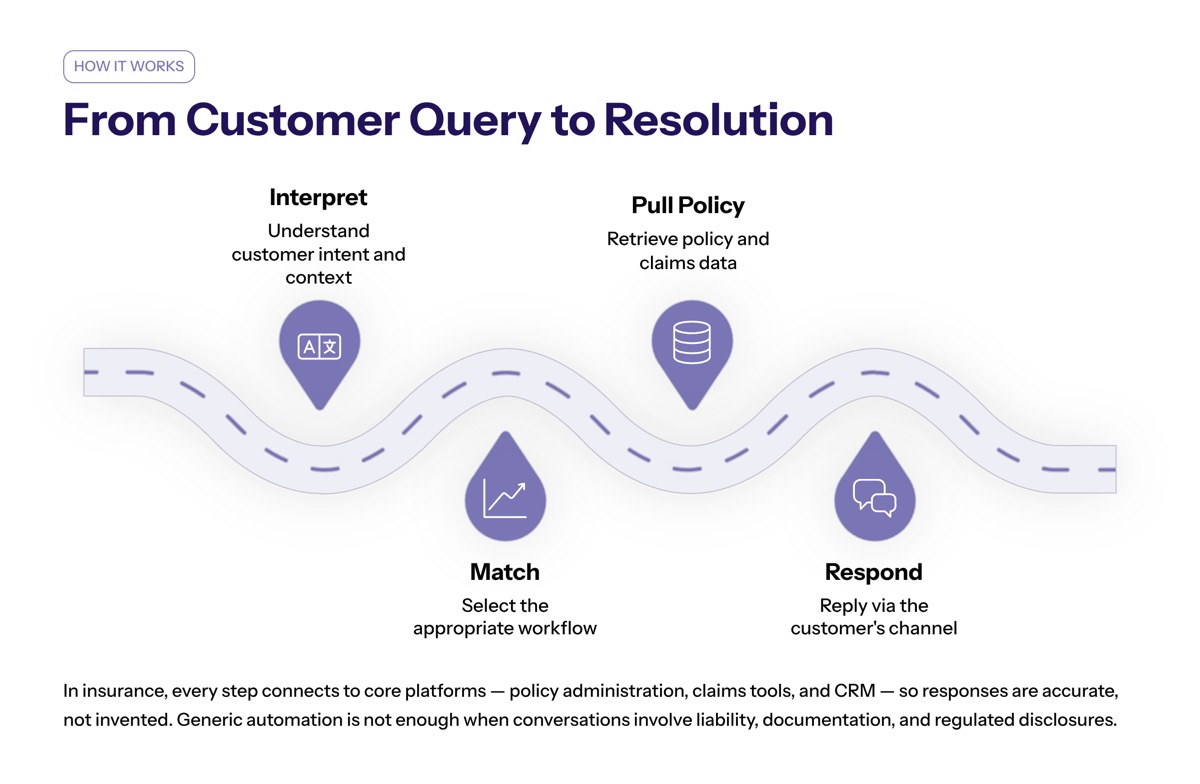
Conversational AI works by interpreting human language, matching the request to an approved workflow, pulling relevant policyholder data, and responding through the right channel. In insurance, this often means connecting the conversational AI platform to core platforms, policy administration platforms, claims tools, and CRM records.
The system may ask structured questions, verify identity, pull data from existing systems, summarize the complete conversation history, and route the case to human customer service representatives when needed. That flow is especially useful when customer calls spike after storms, billing changes, renewal periods, or catastrophe events.
The right conversational AI platform should be designed around insurance-specific workflows. Generic automation is rarely enough because insurance conversations involve liability, documentation, policy language, risk review, and regulated disclosures.
Why the Insurance Industry Is Moving Toward AI
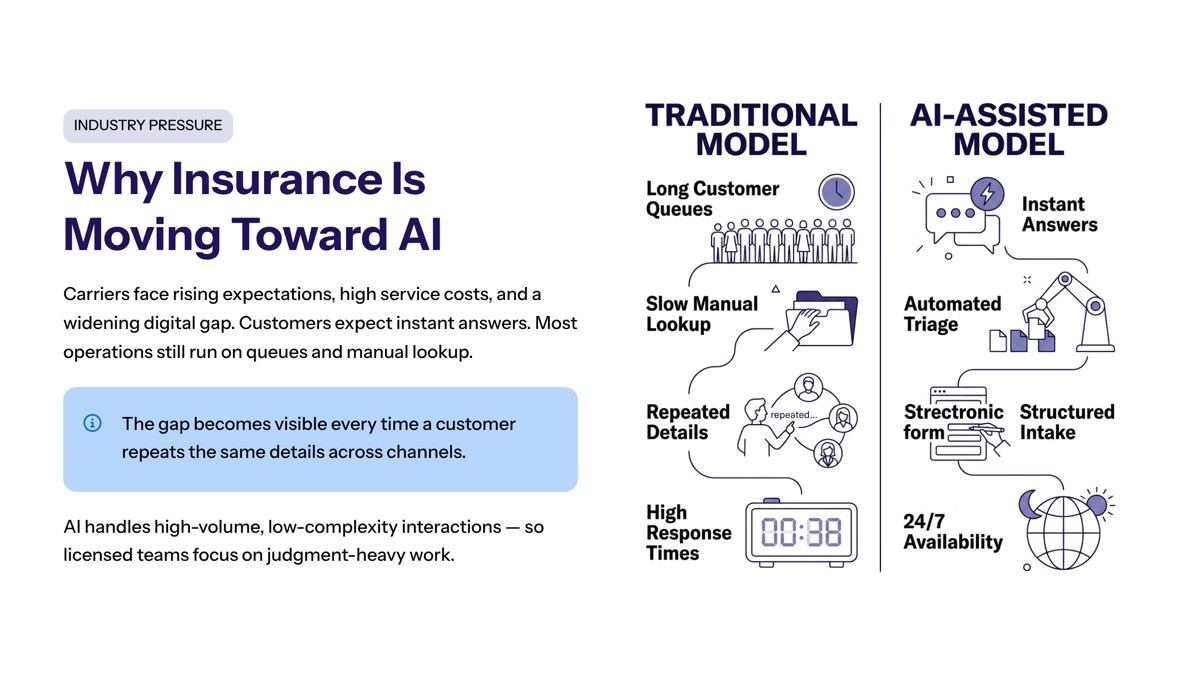
The insurance industry is under pressure from rising customer expectations, high service costs, complex products, and uneven digital experiences. Policyholders expect instant answers, but many insurance companies still depend on traditional customer service models built around queues, transfers, and repeated manual lookup. In the insurance industry, that gap becomes visible every time a customer has to repeat the same details across channels.
AI gives carriers a way to handle high-volume, low-complexity interactions without adding proportional staffing. That matters because customer service teams often spend a large share of their time on routine tasks that do not require deep judgment.
Conversational AI in insurance is not just an upgrade to the front end. It changes how insurance leaders deliver service across claims, policy support, underwriting handoffs, and retention workflows.
Where Conversational AI Creates the Most Value
The highest-value use cases are not vague automation ideas. They are specific workflows where conversational AI can understand customer queries, handle customer queries, collect the right information, and either resolve the issue or escalate cleanly.
For insurance providers, the best starting points are usually policy inquiries, FNOL workflows, billing questions, renewal reminders, claim status requests, and document collection. These interactions are common, measurable, and structured enough for automation.
The goal is not to remove human agents from customer relationships. It is to let service teams spend less time on repetitive lookup and more time on exceptions, complex claims, and retention.

Instant Answers for Policy Inquiries and Coverage Questions
Policy inquiries are a natural fit for conversational AI in insurance. Customers often ask about deductibles, coverage limits, premium changes, renewal dates, payment status, and policy details.
Conversational AI can provide immediate answers when the policy language and customer data are available through approved systems. It can also identify when the question is too sensitive, ambiguous, or risky for automation.
That distinction matters. An insurance policy is a legal and financial document. Conversational AI solutions should provide approved information, not invent interpretations or make coverage promises beyond the policy record. The same principle applies to AI agents that operate across more than one service step.

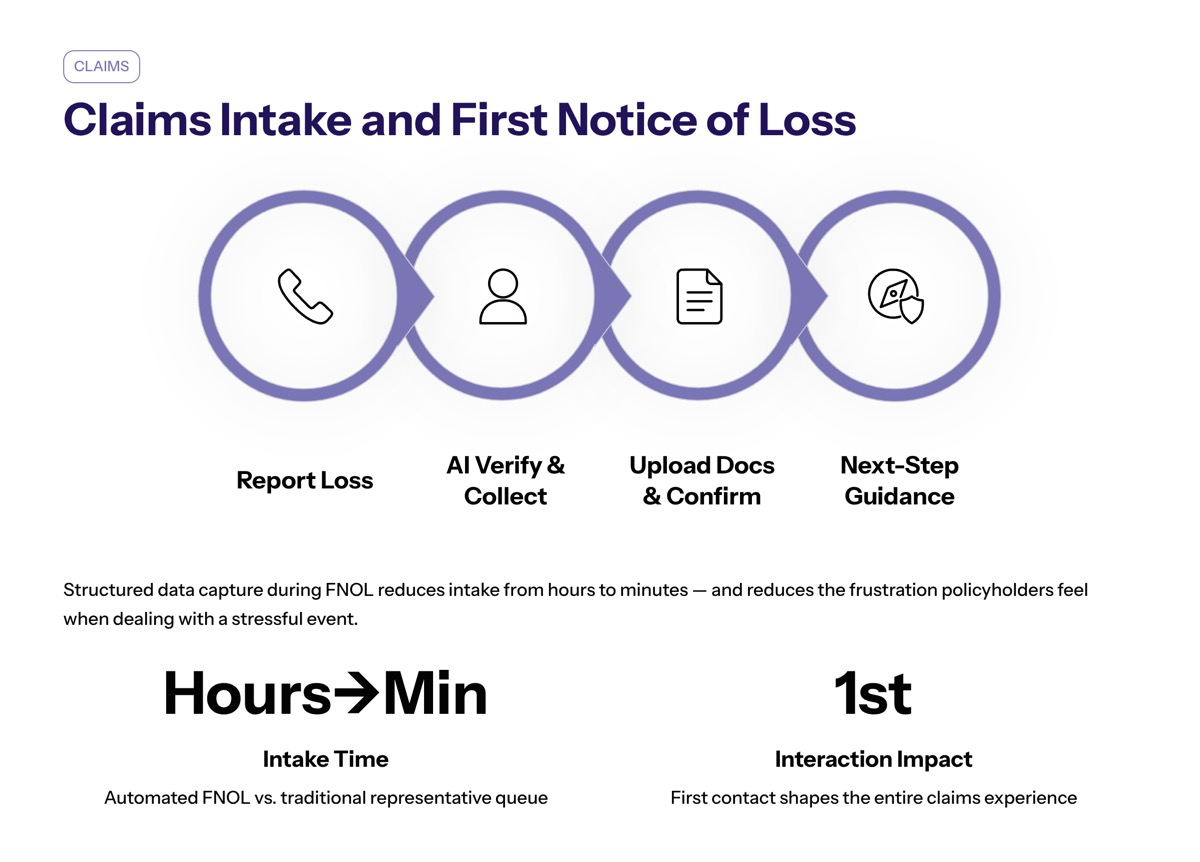
Claims Intake and First Notice of Loss
Claims intake is one of the strongest use cases for insurance conversational AI. When a policyholder reports an accident, property loss, health insurance issue, or other insurance claim, the first interaction shapes the customer experience.
Conversational AI can reduce claims intake times from hours to minutes by automating structured data capture during the First Notice of Loss (FNOL), which significantly improves operational efficiency. Instead of waiting for a representative, the customer can provide incident details, upload documents, confirm contact information, and receive next-step guidance.
Automating structured data capture during First Notice of Loss (FNOL) reduces intake times from hours to minutes, allowing claims teams to start processing sooner. Faster intake reduces the frustration policyholders feel when they are already dealing with a stressful event.
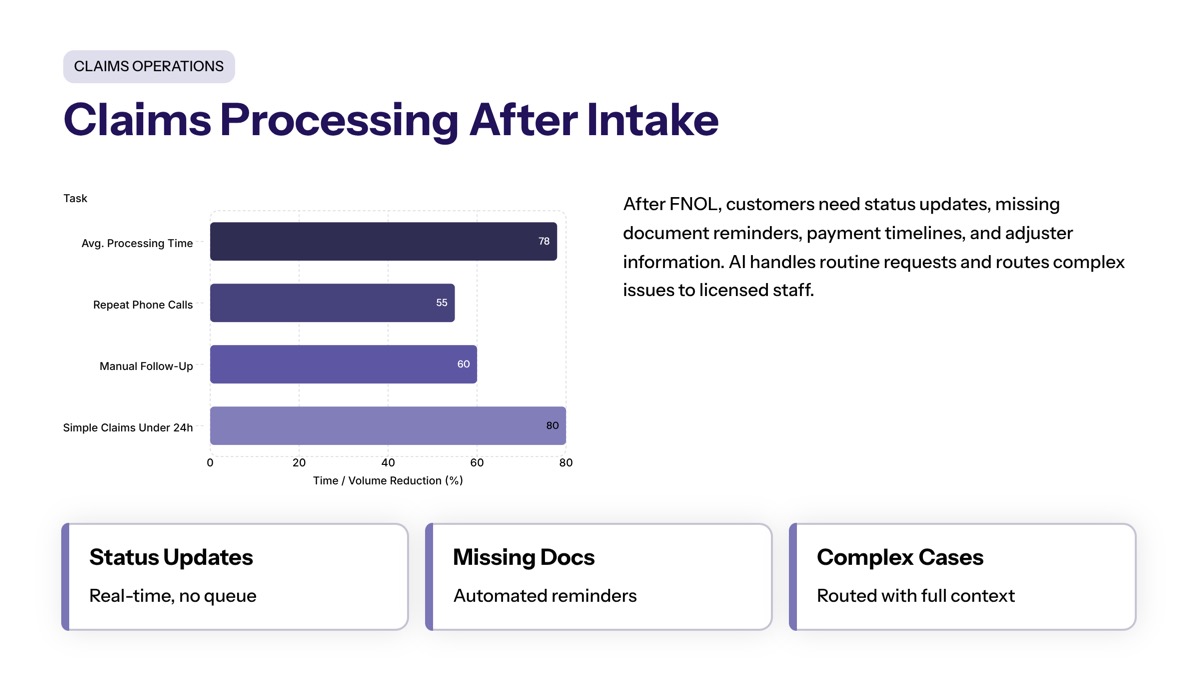
Claims Processing After Intake
Claims processing does not end with initial intake. Customers often want status updates, missing document reminders, payment timelines, adjuster information, and clarification about next steps.
Conversational AI in insurance answers routine claim status questions and routes complex issues to licensed staff. It can also help customers understand what information is still missing, which reduces repeat phone calls and fragmented follow-up.
AI-powered systems can reduce the average claims processing time by up to 78%, with simple claims completed in under 24 hours, significantly improving operational efficiency. That type of result depends on workflow design, integration quality, and the complexity of the insurance claim.
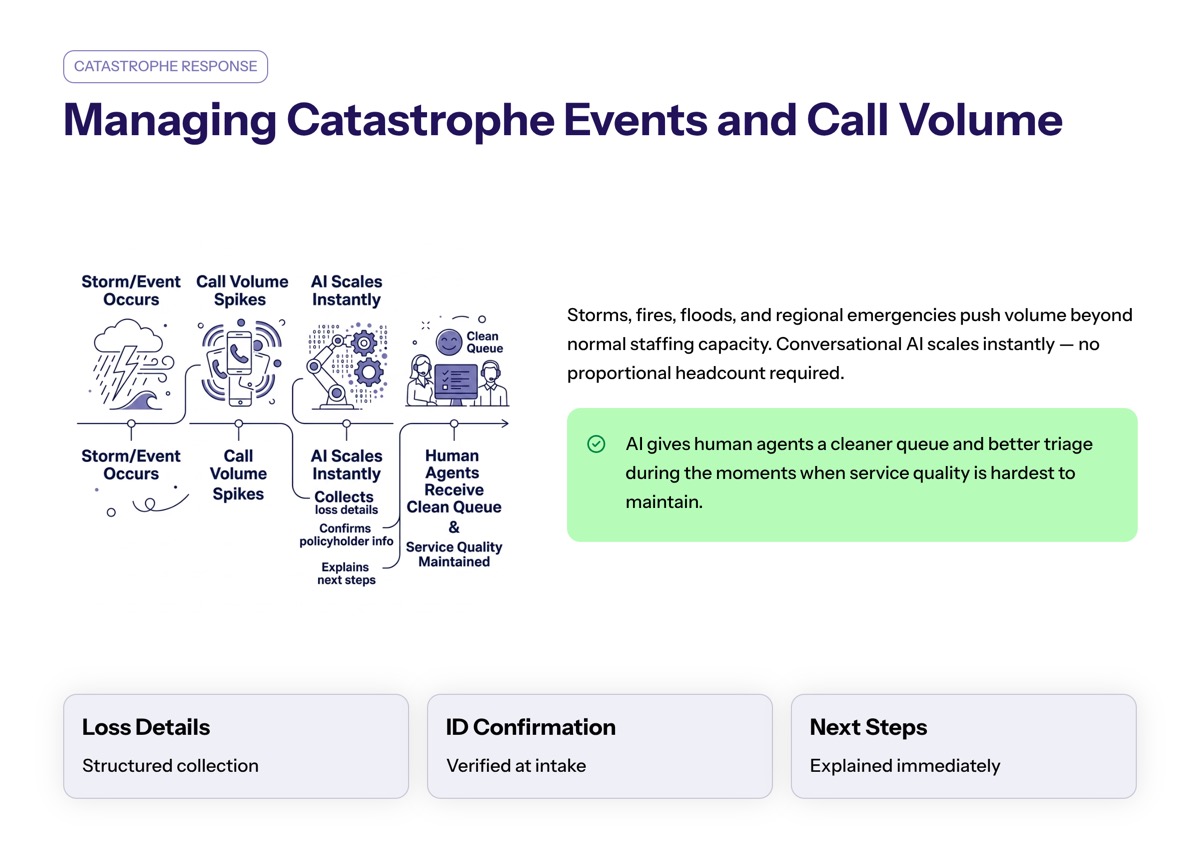
Managing Catastrophe Events and Call Volume
Catastrophe events create sudden spikes in call volume. Storms, fires, floods, and regional emergencies can push customer calls beyond what normal staffing models can absorb.
Conversational AI can scale instantly to manage spikes in claims volume during catastrophe events, providing immediate responses and reducing wait times for policyholders. AI voice agents and messaging assistants can also collect loss details, confirm policyholder information, and explain what happens next.
This does not remove the need for licensed support. It gives human agents a cleaner queue and better triage during moments when service quality is hardest to maintain.
AI Voice Agents for Insurance Service
Voice agents are especially relevant because many policyholders still prefer phone calls for urgent or sensitive insurance conversations. AI voice agents can answer common questions, authenticate callers, collect information, and route the conversation based on urgency.
AI powered voice agents can also help insurance providers handle after-hours requests, weekend spikes, and routine customer calls outside normal business hours. That gives customers more immediate support without forcing every request into the same daytime queue.
The quality bar is high. If automated phone assistants misunderstand customer queries, interrupt callers, or fail to escalate correctly, they can damage customer experience faster than a weak chat assistant.

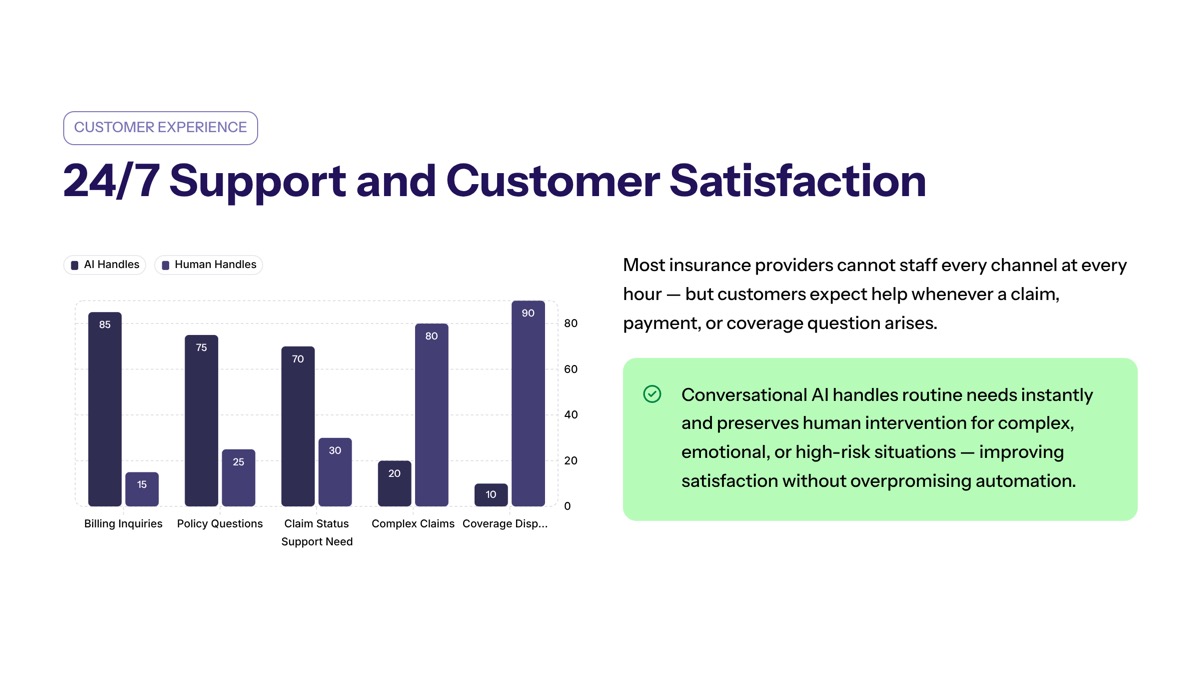
Customer Satisfaction and 24/7 Support
Conversational AI can enhance customer experience by providing 24/7 instant support. Policyholders can receive immediate responses to billing inquiries, policy questions, claim status requests, and other insurance services without waiting on hold.
This is where customer expectations and operational reality meet. Many insurance providers cannot staff every channel at every hour, but customers still want help when a claim, payment issue, or coverage question appears. A strong system can handle customer interactions across channels while keeping escalation visible.
Conversational AI in insurance can provide fast answers for routine needs and preserve human intervention for complex, emotional, or high-risk situations. That balance can improve customer satisfaction without overpromising automation.
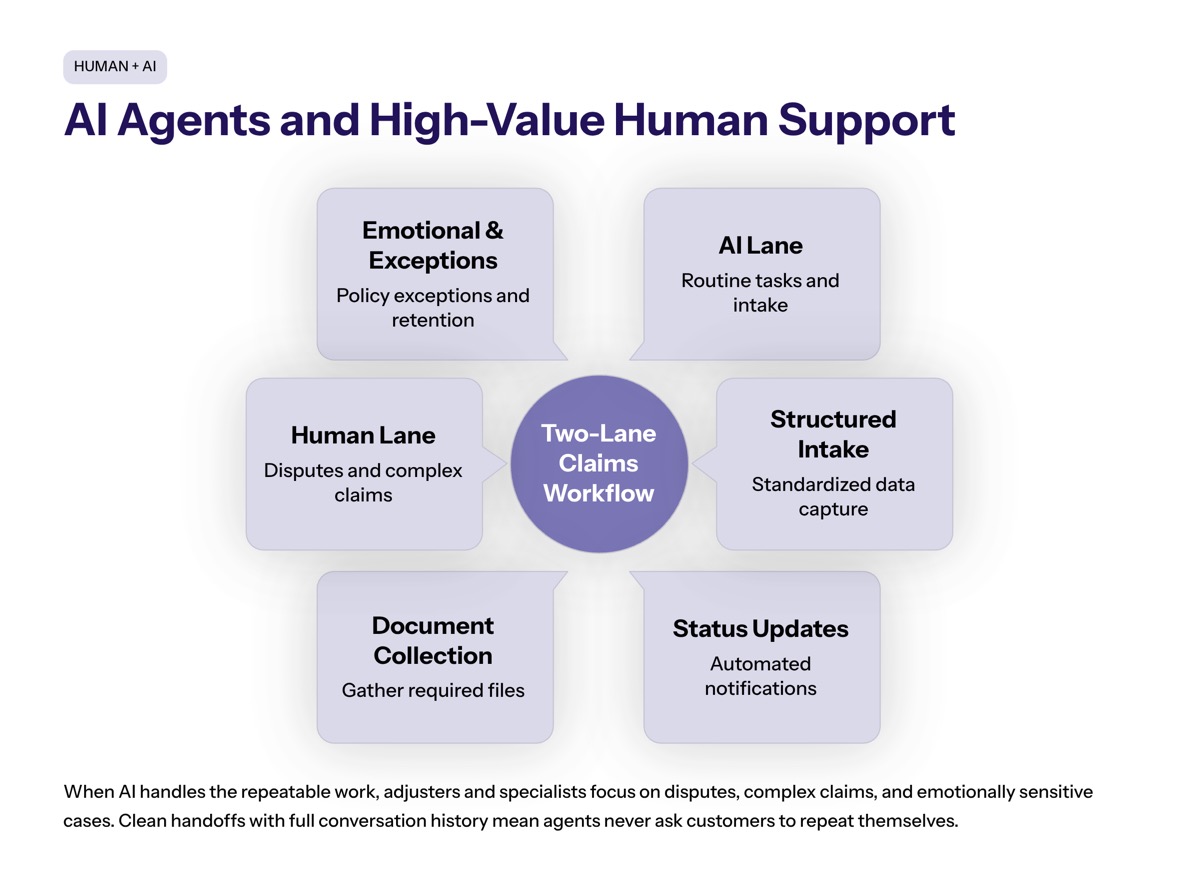
AI Agents and High-Value Human Support
The strongest insurance customer service model is not AI instead of people. It is conversational AI plus human agents working with clearer roles.
When conversational AI handles routine tasks, adjusters and service specialists can focus on disputes, complex claims, policy exceptions, retention conversations, and emotionally sensitive cases. That improves agent performance because the human team spends more time on work that actually needs human judgment.
Human insurance agents also benefit from better handoffs. When the assistant provides complete conversation history, the agent does not have to ask the customer to repeat the same information.
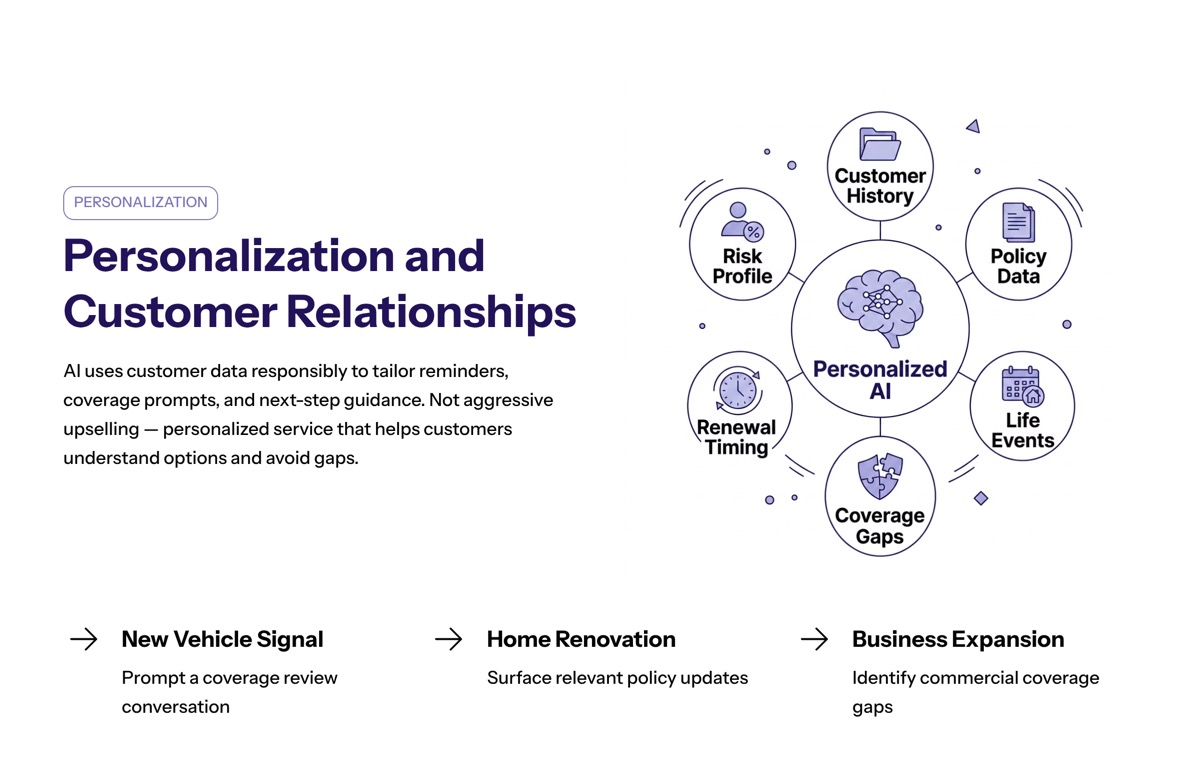
Personalization and Customer Relationships
Conversational AI can improve customer relationships when it uses customer data responsibly. Instead of treating every policyholder the same, the system can tailor reminders, coverage prompts, and next-step guidance around customer needs.
AI systems improve data collection from conversations, leading to better risk assessment and personalized product offerings. For example, a customer asking about a new vehicle, home renovation, or business expansion may need a coverage review.
The goal is not aggressive upselling. The goal is personalized service that helps insurance customers understand policy options and avoid gaps.
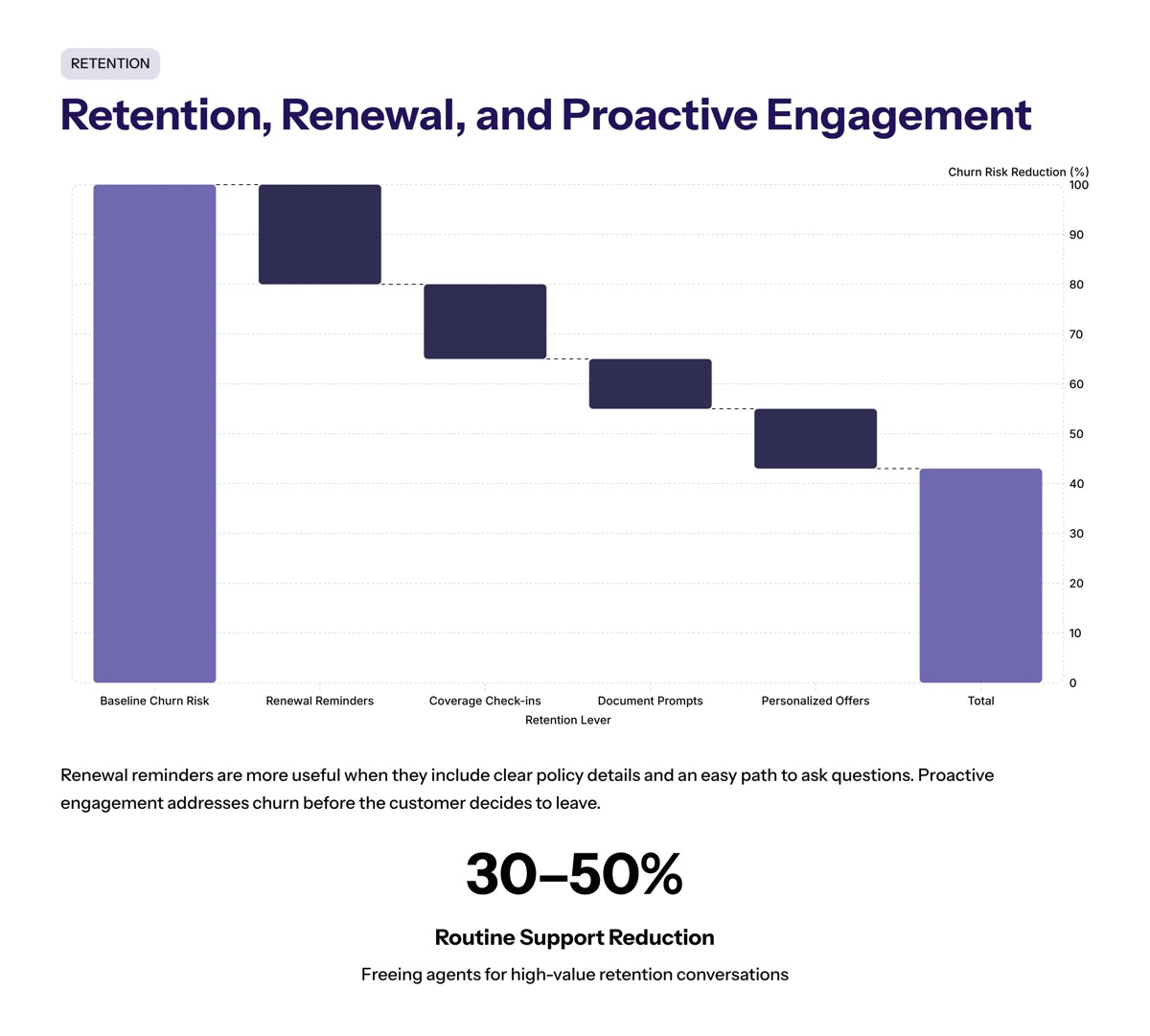
Retention, Renewal, and Proactive Engagement
Retention is a practical use case for conversational AI in insurance. Renewal reminders, coverage check-ins, document prompts, and personalized coverage recommendations can help insurance companies address churn risks before a customer leaves.
Conversational AI can enhance customer retention by providing personalized interactions, such as tailored product recommendations based on individual customer needs and preferences, which increases the likelihood of sales. A renewal reminder is more useful when it includes clear policy details and an easy path to ask questions.
Insurance companies that implement conversational AI report a 30-50% reduction in routine support volume, which allows human agents to focus on more complex, high-value interactions that improve customer retention.
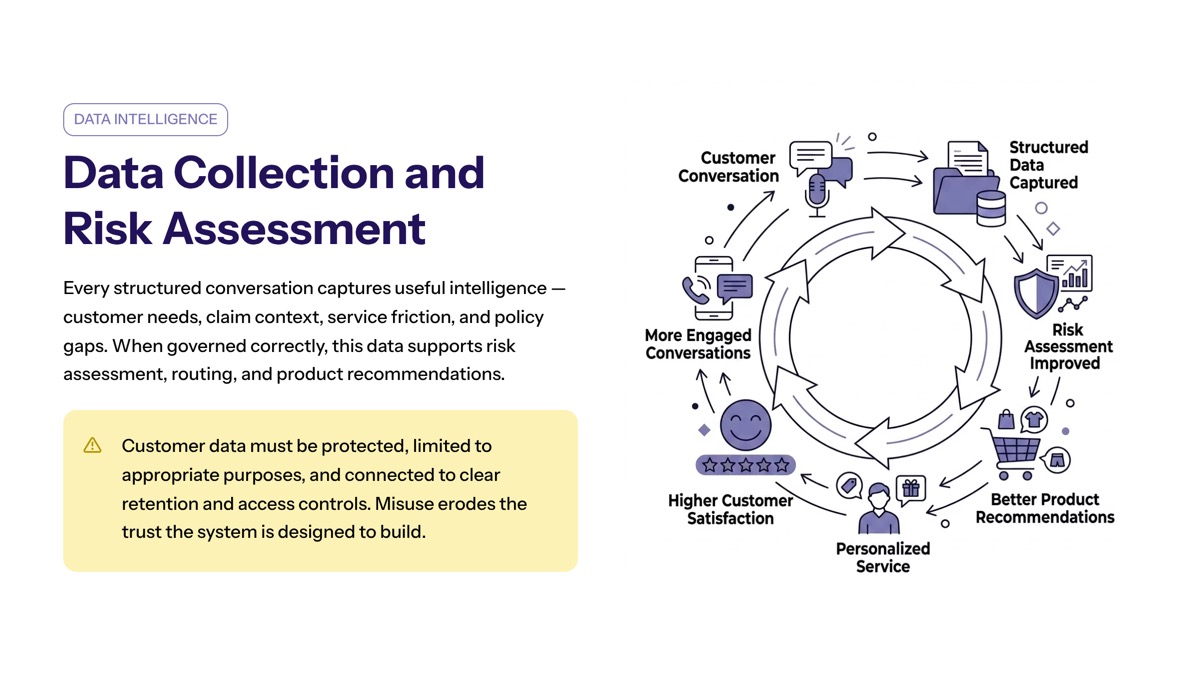
Data Collection and Risk Assessment
Data collection is one of the hidden advantages of conversational AI in insurance. Every structured conversation can capture useful information about customer needs, claim context, service friction, and policy gaps.
When governed correctly, this data can support risk assessment, claims routing, product recommendations, and customer engagement planning. It can also help insurance firms identify repeated service issues that are creating unnecessary contact volume. For the insurance sector, that makes conversation design part of operating intelligence, not only customer service.
The risk is misuse. Customer data must be protected, limited to appropriate purposes, and connected to clear retention and access controls.
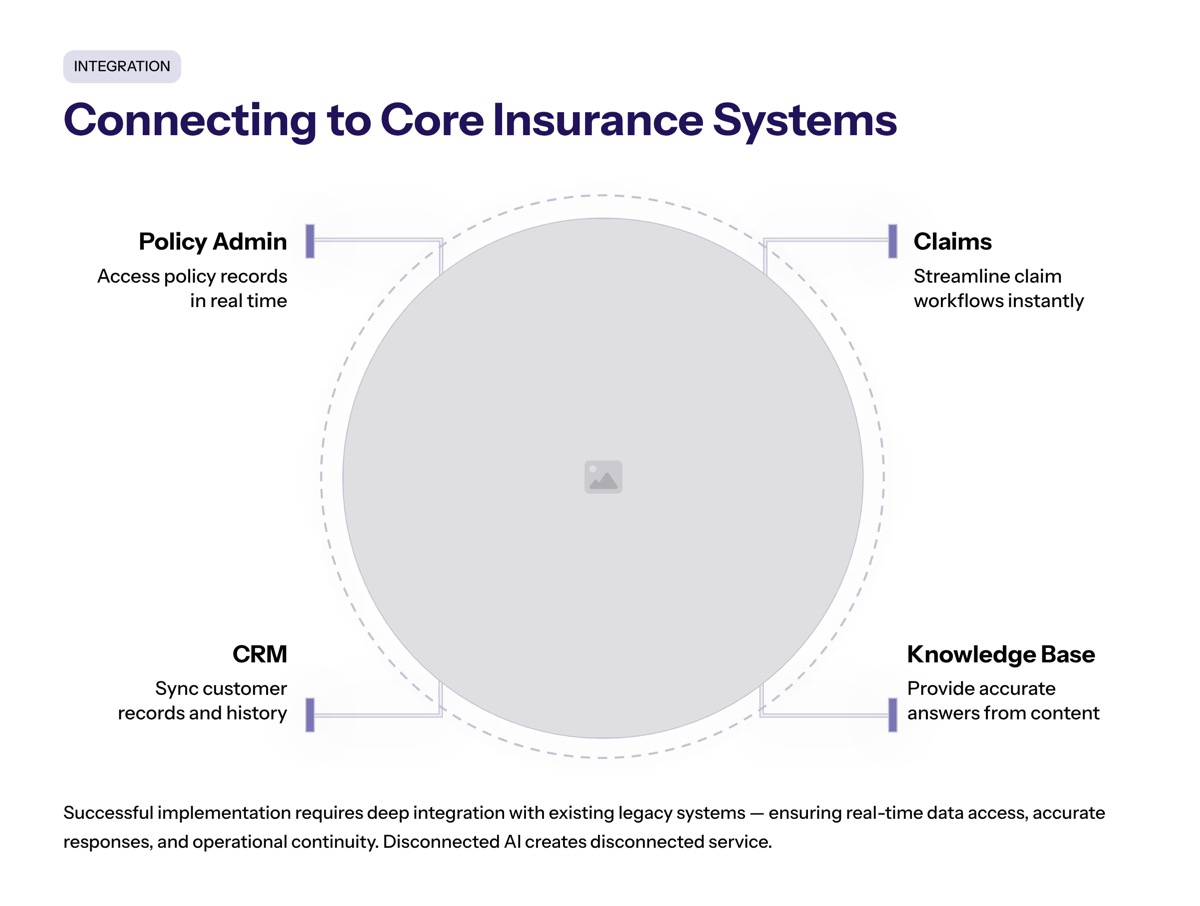
Core Insurance Systems and Existing Systems
Conversational AI in insurance integrates directly with core systems such as policy administration, claims management, and CRM platforms, allowing for real-time data access and improved operational workflows.
Successful implementation of conversational AI in insurance requires integration with existing legacy systems to ensure seamless data flow and operational efficiency, reducing the risk of misinformation and enhancing service delivery.
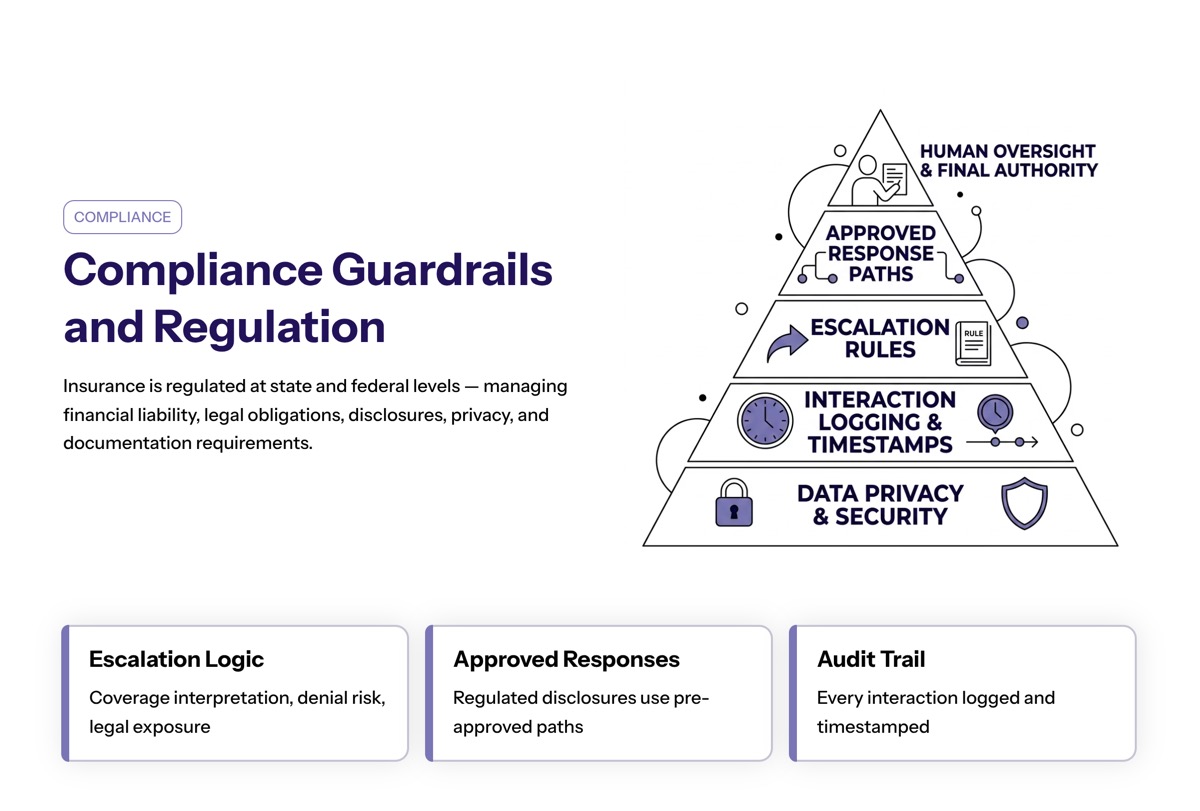
Compliance Guardrails and Regulation
The insurance sector is regulated at both state and federal levels. Insurance companies must manage financial liability, legal obligations, disclosures, privacy rules, and documentation requirements.
Conversational AI systems must include compliance guardrails, escalation logic, and human oversight. If a question involves coverage interpretation, denial risk, legal exposure, or regulated disclosure, the system should escalate or use an approved response path.
Every interaction handled by conversational AI in insurance should be logged and timestamped. That creates an auditable trail that supports regulatory documentation without adding extra manual work.
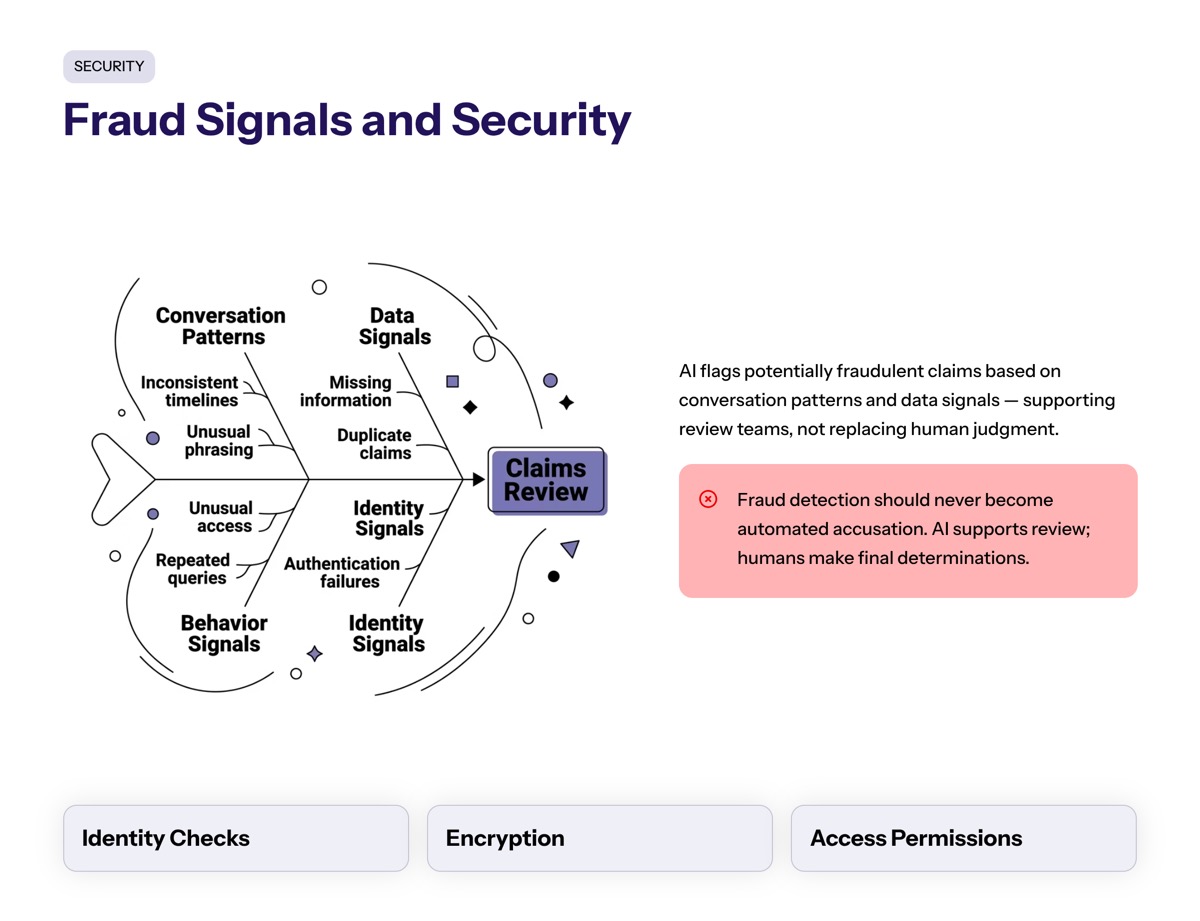
Fraud Signals and Security
AI tools can enhance security by flagging potentially fraudulent claims based on conversation patterns and data signals. This can support claims teams by identifying inconsistencies, unusual behavior, or missing information earlier in the process.
Fraud detection should not become automated accusation. The role of conversational AI technology is to support review, not make final determinations without human oversight.
Security also applies to access. Any conversational AI platform handling policy details, claims documents, or customer data needs identity checks, permissions, encryption, monitoring, and incident response planning.
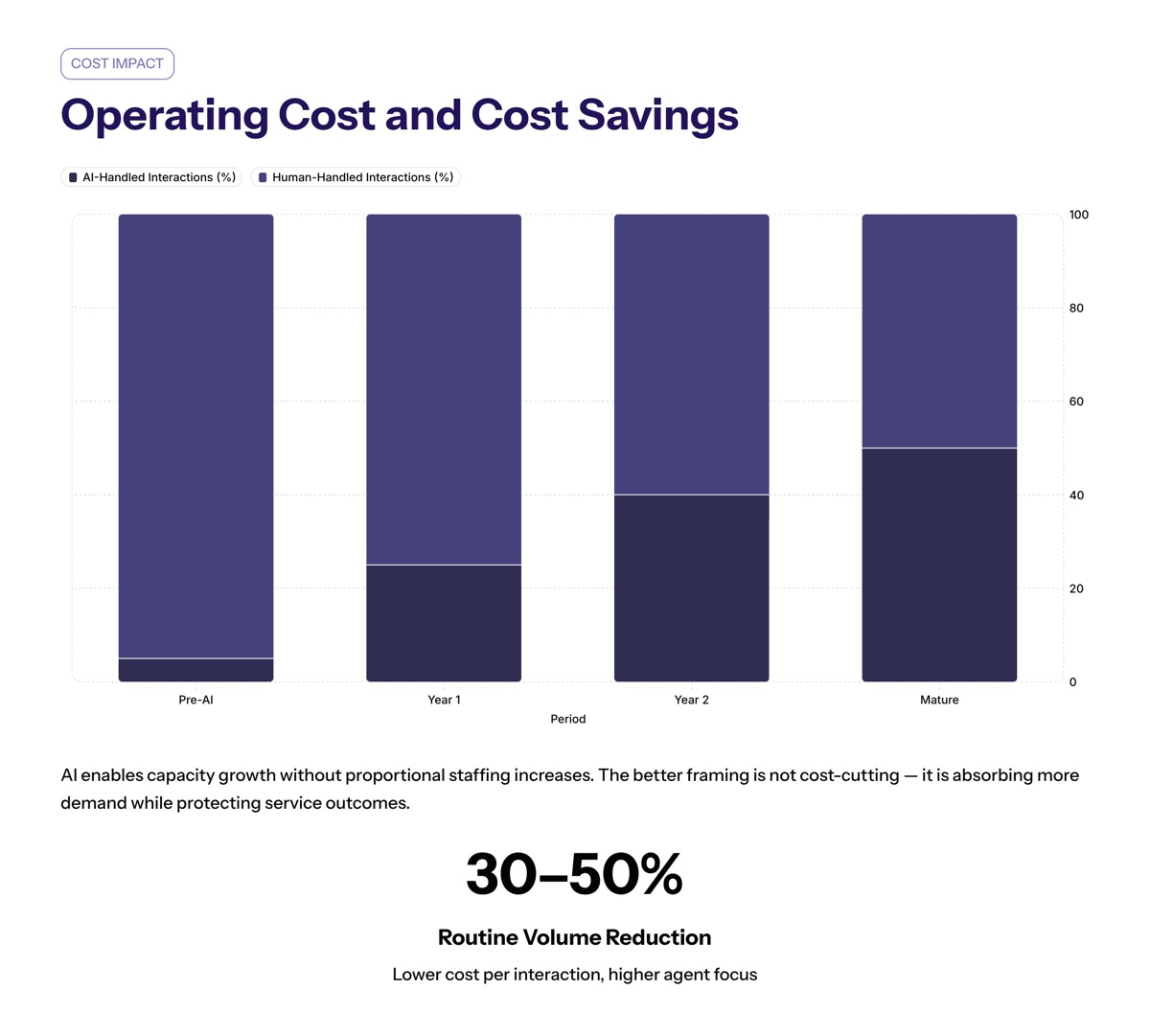
Operating Cost and Cost Savings
The implementation of conversational AI in insurance can significantly reduce operational costs by automating routine customer inquiries, which allows human agents to focus on more complex and high-value interactions.
Automation of routine tasks significantly reduces staffing needs and operational costs in the insurance industry, but the better framing is capacity management. Insurance companies can absorb more demand while protecting service outcomes.
Insurance companies that implement conversational AI typically see a 30-50% reduction in routine support volume, leading to lower operational costs and improved efficiency. Automating routine inquiries with conversational AI can lower the cost per interaction, allowing insurance companies to handle high-volume, low-complexity interactions without proportional staffing increases, thus optimizing operations.
How AI Enhances Customer Experience
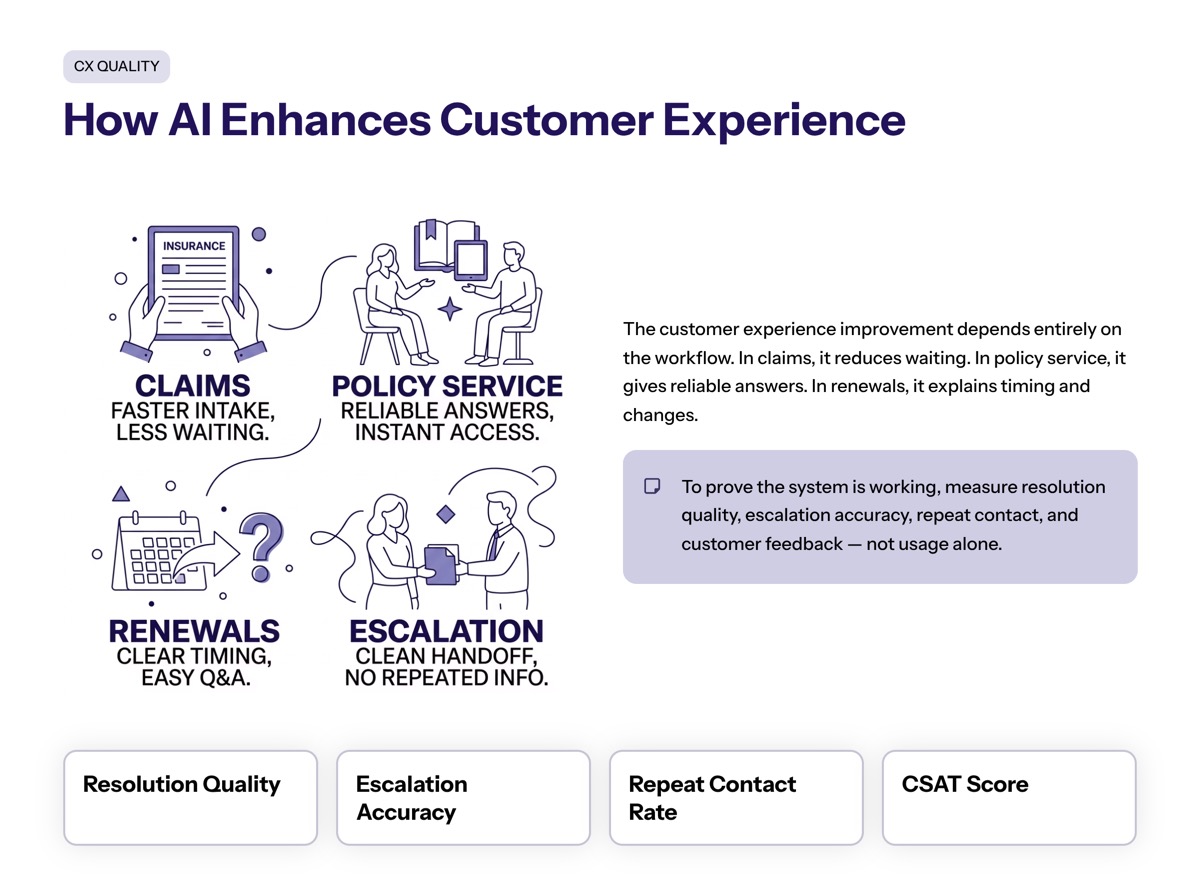
How conversational AI improves the customer experience depends on the workflow. In claims, it reduces waiting and speeds up structured intake. In policy service, it gives reliable answers faster. In renewals, it helps customers understand timing, changes, and next steps.
Conversational AI can enhance customer experience when it resolves routine needs quickly and hands off complex needs cleanly. That is especially important in insurance because many customer interactions happen during stressful moments.
To enhance customer experience, operating teams should measure resolution quality, escalation accuracy, repeat contact, and customer feedback. Usage alone does not prove the system is working.
How Conversational AI Supports Insurance Agents
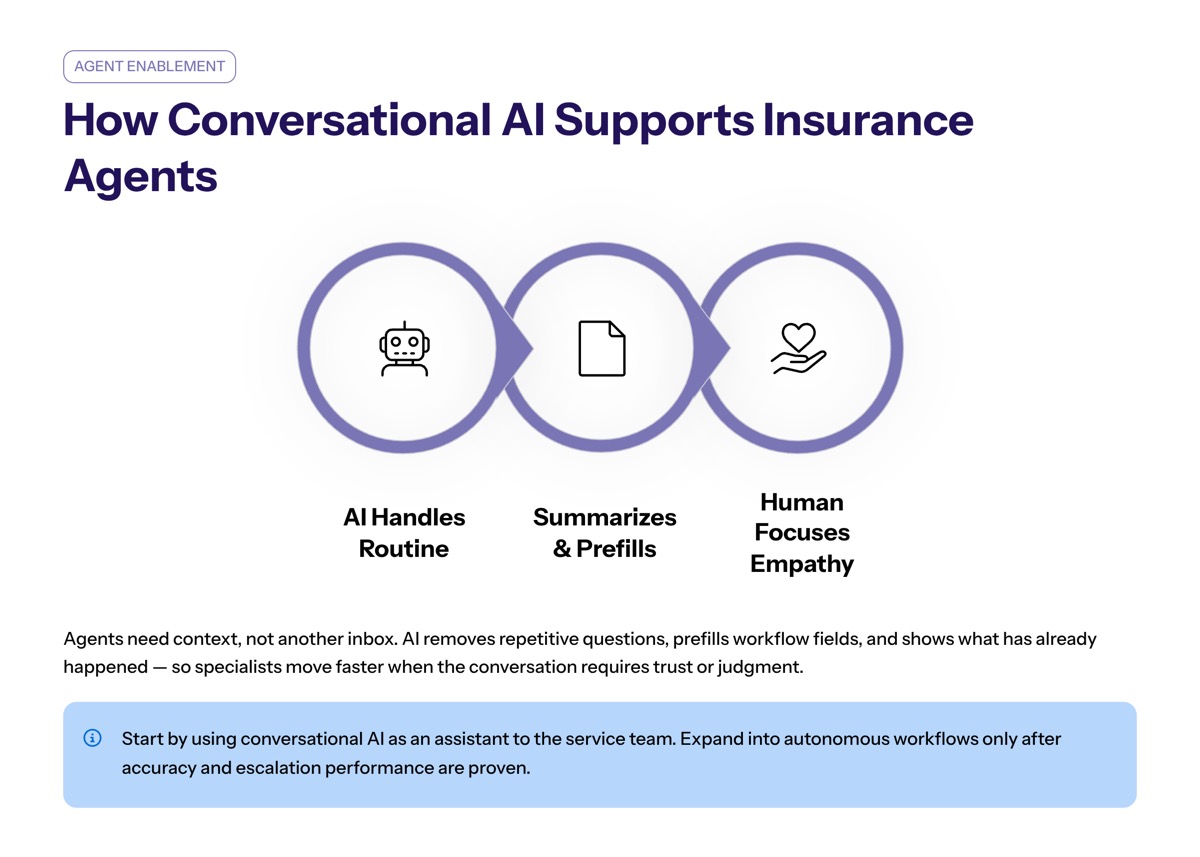
Insurance agents need context, not another inbox. Conversational AI can summarize customer interactions, collect missing information, prefill workflow fields, and show what has already happened before the agent joins.
This helps human agents avoid repetitive questions and focus on customer trust. It also helps human customer service representatives move faster when the conversation requires empathy or judgment.
Many insurance providers should start by using conversational AI as an assistant to the service team, then expand into more autonomous workflows only after accuracy and escalation performance are proven.
Example of Conversational AI in Insurance
An example of conversational AI is a claims assistant that receives a policyholder's loss report after a storm. The assistant verifies identity, collects the date and location of loss, asks for photos, confirms the insurance policy, and explains the next step.
If the claim is simple, the system may complete the intake and trigger the first claims processing workflow. If the case is complex, emotional, or unclear, it routes the customer to a licensed representative with the full conversation history attached.
This kind of workflow is more useful than a generic ai customer service agent because it is designed around insurance operations and connected to claims operations.

What Are the 5 C's of Insurance?
The phrase "5 C's of insurance" can vary by source and context, so insurance providers should define it clearly if they use it in customer education. In a service context, the useful version is coverage, cost, claims, compliance, and customer care.
Coverage explains what the insurance policy does and does not cover. Cost explains premiums, deductibles, and payment expectations. Claims explains how an insurance claim moves from intake to resolution.
Compliance addresses regulated communication and documentation. Customer care covers the service experience across channels, human support, phone support, and digital support.

How AI Is Being Used in the Insurance Industry
AI in insurance is used for claims triage, document processing, fraud signal detection, risk review, customer service, underwriting support, renewal engagement, and workflow automation.
Conversational AI in insurance is the customer-facing part of that larger AI in insurance stack. It handles insurance conversations, collects data, answers questions, and coordinates handoffs across service and claims workflows.
The insurance market is likely to keep adopting AI where it improves speed, consistency, and service quality. The constraint is governance: AI must fit regulated insurance operations, not bypass them. That is why AI in insurance should be treated as artificial intelligence inside a controlled workflow, not as an unmanaged response layer.
Is Conversational AI in Healthcare the Same Thing?
Conversational AI in healthcare and conversational AI in insurance share some foundations, including natural language processing, virtual assistants, escalation, and secure data handling. The operating context is different.
Healthcare workflows focus on patient access, care navigation, clinical workflow, and patient safety. Insurance workflows focus on policy service, FNOL, claims processing, customer experience, and regulated financial obligations.
The overlap matters because health insurance sits between both worlds. A health insurance conversational AI system may need to handle coverage details, provider networks, claims questions, and sensitive customer data without drifting into medical advice.
Choosing a Comprehensive Conversational AI Solution
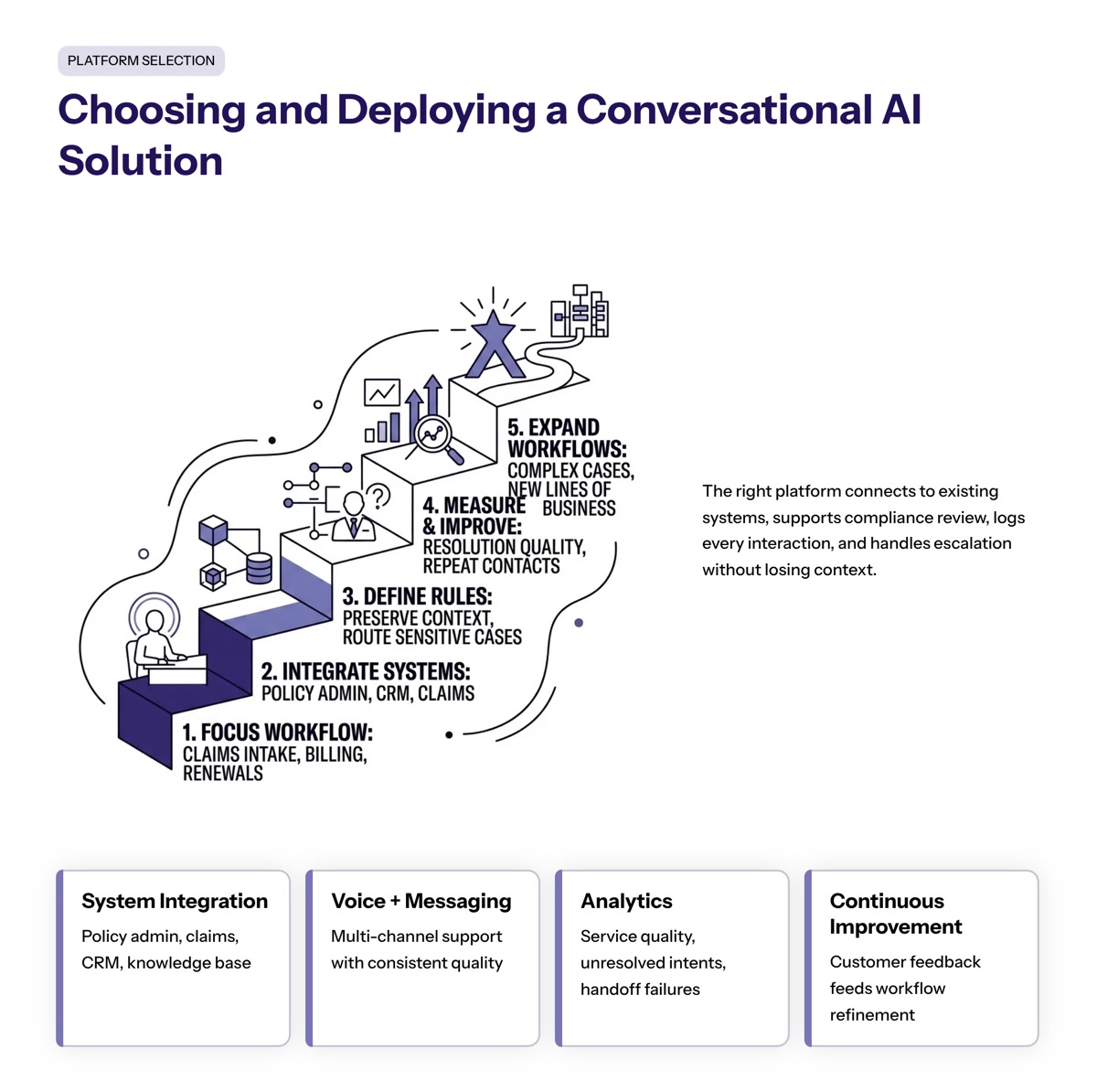
The right conversational AI platform for insurance should connect to existing systems, support compliance review, log interactions, and handle escalation without losing context.
Insurance executives should evaluate whether the platform can understand customer queries, manage customer data securely, support voice automation and messaging platforms, and provide analytics on service quality.
A comprehensive conversational AI solution should also help teams improve workflows over time. Customer feedback, unresolved intents, repeat contacts, and handoff failures should become inputs for continuous improvement.
Deploy Conversational AI Without Creating New Risk
To implement conversational AI safely, insurance companies should start with a focused workflow. Claims intake, service questions, renewal reminders, and billing questions are usually better starting points than complex coverage interpretation.
The next step is integration. The conversational AI system should connect to core platforms, claims management, CRM tools, and knowledge sources so it can provide accurate answers and avoid disconnected service.
Finally, define escalation. If the assistant cannot answer confidently, detects risk, or receives a sensitive request, it should move the conversation to licensed staff with context preserved.
Metrics Insurance Leaders Should Track
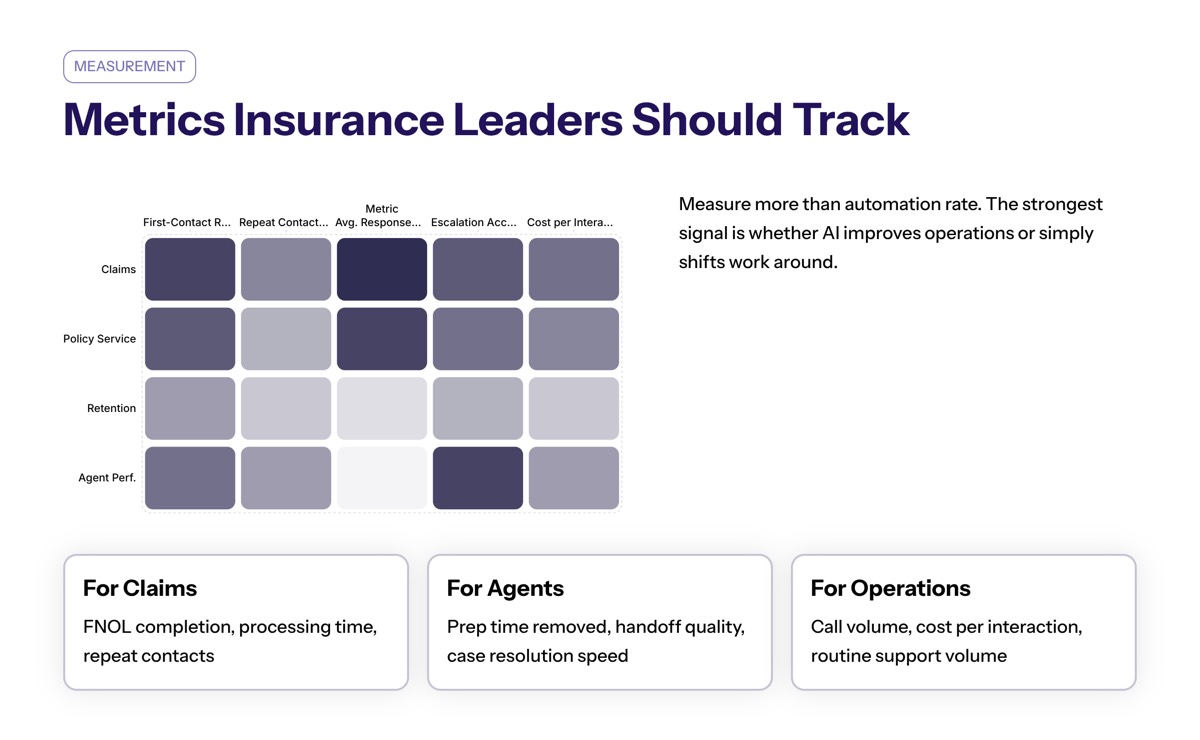
Operating teams should measure more than automation rate. Useful metrics include first-contact resolution, repeat contact rate, average response time, escalation accuracy, FNOL completion, policy inquiry resolution, and customer satisfaction.
For agent performance, track how much prep work conversational AI removes, how often handoffs include complete context, and whether specialists can resolve complex cases faster.
For operational efficiency, track call volume, cost per interaction, claims processing time, routine support volume, and quality outcomes. These metrics show whether AI in insurance is improving operations or only shifting work around.
Where Insurance Teams Should Start
Insurance teams should start where the workflow is structured, measurable, and painful for both customers and staff. Claims intake, policy questions, billing questions, renewal reminders, and claim status updates are usually stronger starting points than open-ended coverage advice.
That approach gives leaders a controlled way to test accuracy, escalation, integration, and customer response before expanding conversational AI into more complex insurance operations.
Final Takeaway
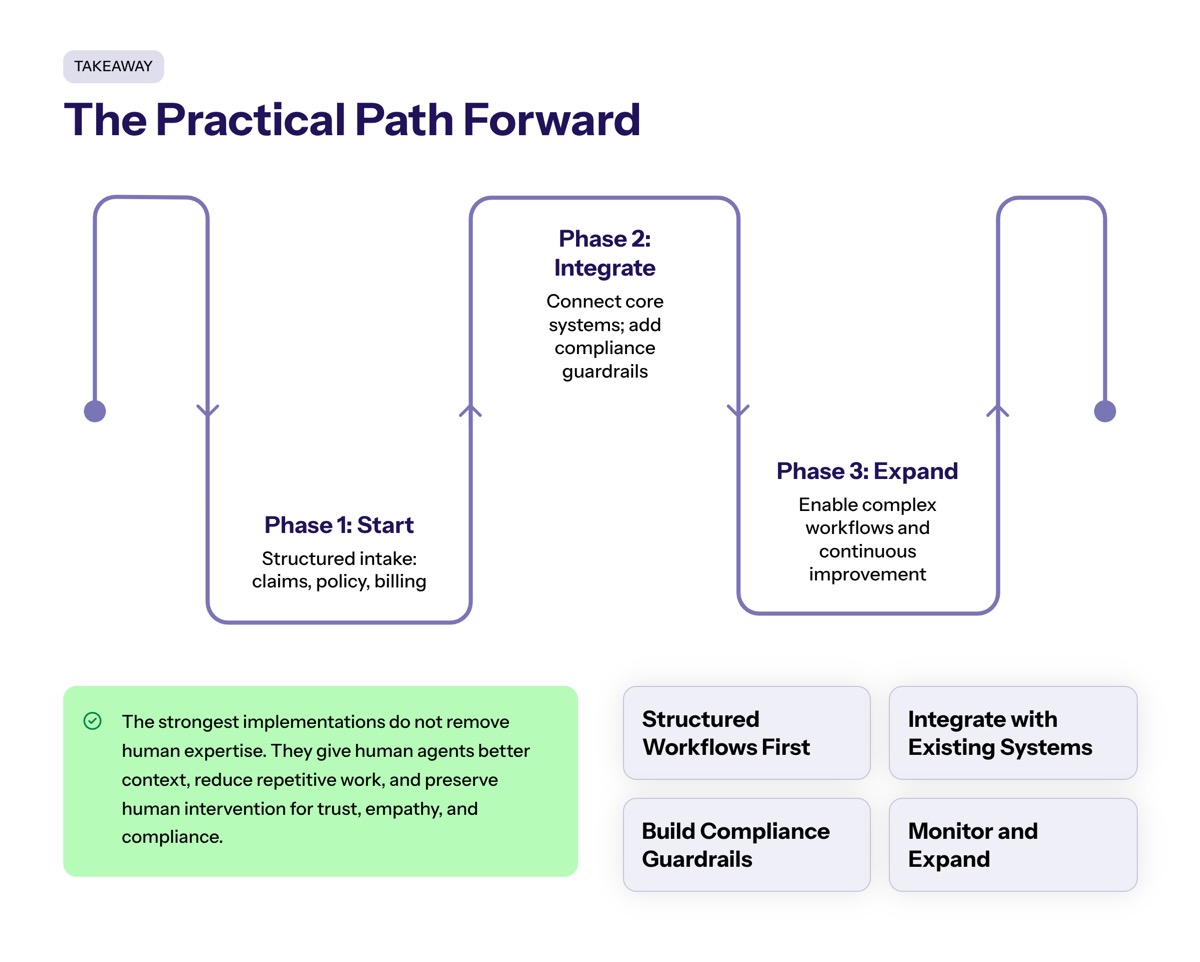
Conversational AI in insurance improves structured intake, reduces routine support volume, lowers cost pressure, and enhances customer experience when it is connected to real insurance operations.
The strongest implementations do not remove human expertise. They give human agents better context, reduce repetitive work, and preserve human intervention for the situations where trust, empathy, judgment, and compliance matter most.
For insurance companies, the practical path is clear: start with structured workflows, integrate with existing systems, build compliance guardrails, monitor customer feedback, and expand only when service metrics improve.